Image Source: https://shorturl.at/85fwX
Moyamoya Disease (MMD) is a rare and complex cerebrovascular condition that uniquely challenges patients and medical professionals. This guide aims to help you understand Moyamoya Disease, from its causes, symptoms, and diagnosis, to treatment options and ongoing research.
What is Moyamoya Disease?
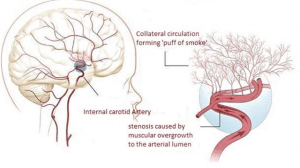
Moyamoya Disease is a rare blood vessel disorder. Moyamoya disease is characterized by a progressive narrowing of the internal carotid arteries and their branches. Ideally, Carotid arteries play a huge role in supplying the blood to the brain. In Moyamoya’s case, these arteries become stenosed (narrowed), making it difficult for them to avail blood to the parts of the brain.
In other words, this means that the blood supply to the brain is compromised. This compromises the brain’s blood supply. To increase the chances of survival in human beings, the brain attempts to compensate for this reduced supply. The brain does this by developing a network of small, fragile blood vessels at its base.
When these abnormal vessels are visualized on an angiogram, they resemble a cloud or puff of smoke, which is what “Moyamoya” describes in Japanese. This name was chosen because of the characteristic appearance seen on angiograms (imaging studies of blood vessels) in patients with the disease. This narrowing reduces the blood flow to critical areas of the brain, making individuals more susceptible to strokes, transient ischemic attacks (TIAs), and other neurological complications.
Stages of Moyamoya Disease (Suzuki Staging System)
- Stage 1: Narrowing of the Internal Carotid Artery
The initial stage is characterized by the beginning of stenosis (narrowing) of the internal carotid artery at the base of the brain. The lumen (interior space) of the artery becomes narrower, but there are typically no significant compensatory changes yet. Imaging findings show a mild narrowing of the internal carotid artery with no evidence of collateral vessel formation.
- Stage 2: Initiation of Moyamoya Vessels
As the stenosis progresses, the body begins to form small, abnormal collateral vessels around the base of the brain to compensate for reduced blood flow. These vessels are known as “moyamoya” vessels, named after the Japanese term for “a puff of smoke,” reflecting their appearance in angiography. Imaging findings show a more pronounced narrowing of the internal carotid artery with early formation of moyamoya vessels.
- Stage 3: Intensification of Moyamoya Vessels
The stenosis becomes more severe, leading to further development and proliferation of moyamoya vessels. This stage is marked by a peak in the number and density of these abnormal vessels. Imaging findings show a severe narrowing or occlusion of the internal carotid artery with dense networks of moyamoya vessels.
- Stage 4: Minimization of Moyamoya Vessels
As the disease progresses, the compensatory moyamoya vessels begin to diminish in number. The remaining vessels become insufficient to maintain adequate cerebral blood flow. Imaging findings indicate a progressive occlusion of the internal carotid artery with a reduction in the number of moyamoya vessels. The brain begins to develop more external collateral circulation (from external carotid arteries).
- Stage 5: Reduction of Moyamoya Vessels
The moyamoya vessels continue to diminish, leading to a significant reduction in blood flow to the brain. The collateral circulation from external sources becomes more prominent. In this stage, the imaging findings show an almost complete occlusion of the internal carotid artery with a marked reduction in moyamoya vessels. There is significant reliance on external carotid artery collaterals.
- Stage 6: Disappearance of Moyamoya Vessels
The final stage is characterized by the near-total disappearance of moyamoya vessels. By this point, the internal carotid artery is typically completely occluded, and the brain relies entirely on collateral circulation from external sources. The imaging findings show a complete occlusion of the internal carotid artery with the disappearance of moyamoya vessels and prominent external carotid artery collateral circulation.
Clinical Implications of Each Stage
- Stages 1-3. Typically represents the earlier stages of the disease, where there might still be some capacity for the brain to compensate through the development of moyamoya vessels.
- Stages 4-6. Represent more advanced disease, where the compensatory mechanisms are failing, leading to increased risk of strokes, transient ischemic attacks (TIAs), and other neurological symptoms.
Causes of Moyamoya Disease
The exact cause of this condition remains largely unknown. However, several factors scientists believe contribute to the development of Moyamoya disease. They include;
1. Genetic Factors
- Inherited Risk. In some cases, Moyamoya Disease has a genetic component, particularly in East Asian populations. The RNF213 gene mutation has been identified as a significant risk factor, especially in people of Japanese, Korean, and Chinese descent. Families with a history of Moyamoya Disease may have a higher likelihood of developing the condition.
- Sporadic Cases. While genetic factors are significant, many cases of Moyamoya Disease occur sporadically, without a known family history. This indicates that other factors may also play a role.
2. Associated Conditions
- Other Diseases. Moyamoya Disease is associated with other medical conditions such as Down syndrome, neurofibromatosis type 1, sickle cell disease, and certain autoimmune disorders. In these cases, the disease may develop as a secondary condition linked to the underlying health issue.
- Radiation Exposure. There is some evidence that exposure to radiation, particularly in the treatment of brain tumours, may increase the risk of developing Moyamoya Disease later in life.
3. Environmental Factors
- Environmental Influence. While environmental factors are not well understood, they may influence the development of Moyamoya Disease. This is particularly true in individuals who have a genetic predisposition. However, specific environmental triggers have not been definitively identified.
4. Immune System Abnormalities
- Autoimmune Component. Some research suggests that Moyamoya Disease may involve an abnormal immune response. In this, the body’s immune system mistakenly attacks healthy blood vessels in the brain. This theory is supported by the presence of the disease in individuals with other autoimmune conditions.
5. Idiopathic Nature
- Unknown Causes. In many cases, the exact cause of Moyamoya Disease remains unknown, and it is classified as idiopathic. Researchers continue to investigate potential triggers and contributing factors to better understand the disease’s origins.
Symptoms of Moyamoya Disease
The symptoms of Moyamoya Disease vary widely, depending on the age of onset and the severity of the condition. Some common symptoms include:
- Recurrent Strokes. These can cause sudden weakness or numbness in one side of the body, difficulties with speech, or loss of vision. Recurrent strokes are the most severe manifestation and require immediate medical attention.
- Transient Ischemic Attacks (TIAs). TIAs are often described as mini-strokes. They cause brief episodes of stroke-like symptoms that typically resolve within a few minutes to hours. Despite their short duration, TIAs indicate a serious risk for future strokes.
- Headaches. People with Moyamoya disease often complain of severe, persistent headaches that are common and can be debilitating. They may precede other symptoms or occur independently.
- Seizures. Some individuals with Moyamoya Disease experience seizures, which may involve convulsions, loss of consciousness, or unusual sensations.
In children, the signs and symptoms of this disease manifest differently. Children may experience developmental delays or difficulties with motor skills. Detecting this disease is crucial as it helps in managing these symptoms effectively, improving the quality of life.
Diagnosing Moyamoya Disease
Diagnosing Moyamoya Disease involves a combination of medical history, clinical examination, and advanced imaging techniques:
- Magnetic Resonance Imaging (MRI). MRI scans are key tests used for visualizing changes in brain structure and detecting areas of ischemia or infarction. They help identify damage to brain tissue and guide treatment decisions.
- Magnetic Resonance Angiography (MRA). MRA scan provides detailed images of the brain’s blood vessels. They visualise the narrowing of the arteries and the presence of compensatory blood vessels. This imaging technique is less invasive than traditional angiography and is valuable during initial diagnosis.
- Cerebral Angiography. This is the most definitive diagnostic tool for Moyamoya Disease. It involves injecting a contrast dye into the blood vessels and taking X-ray images to visualize blood flow and detect any abnormalities. It clearly shows the characteristic “puff of smoke” appearance of the collateral vessels.
Treatment Options for Moyamoya Disease
Any treatment given for Moyamoya Disease aims to improve blood flow to the brain and prevent further strokes. The approach often involves a combination of medication and surgery as follows:
Medications
1. Antiplatelet Agents
These medications help prevent blood clots, reducing the risk of stroke by keeping blood platelets from sticking together. Examples include:
- Aspirin. A common antiplatelet medication that is often prescribed to Moyamoya patients to reduce the risk of ischemic strokes.
- Clopidogrel (Plavix). Another antiplatelet drug may be used if aspirin is not tolerated or in combination with aspirin.
2. Anticoagulants.
Anticoagulants work by preventing blood clotting, which can help reduce the risk of stroke. This is important, especially in patients with a history of transient ischemic attacks (TIAs) or previous strokes. Examples include:
- Warfarin (Coumadin). This is a commonly used anticoagulant. It requires regular blood monitoring.
- Heparin. This is used in acute settings, particularly during surgery or in the hospital to prevent clot formation.
3. Calcium Channel Blockers.
These medications can help alleviate headaches. They also reduce the frequency of transient ischemic attacks by relaxing blood vessels and improving blood flow to the brain. Examples include:
- Nimodipine (Nimotop). This drug is often used to treat and prevent headaches associated with Moyamoya Disease.
- Verapamil (Calan, Isoptin). This is another calcium channel blocker that may be prescribed for similar purposes.
4. Corticosteroids.
Corticosteroids may be used in some cases to reduce inflammation in the blood vessels and minimise symptoms. Their use is more experimental and not standard for all patients. Examples include:
- Prednisone. This is a commonly prescribed corticosteroid, though its use in Moyamoya is not routine. It is usually reserved for specific cases.
5. Antihypertensive Medications.
These are prescribed for managing high blood pressure in Moyamoya patients. Hypertension can exacerbate the risk of strokes so these drugs help control blood pressure levels. Examples include:
- Lisinopril (Prinivil, Zestril): An ACE inhibitor used to lower blood pressure.
- Amlodipine (Norvasc). This calcium channel blocker is also used to control blood pressure.
6. Anti-seizure Medications.
Some patients with Moyamoya Disease may experience seizures, which need to be controlled with anti-seizure medications. Examples include:
- Levetiracetam (Keppra). This is commonly used to control seizures in Moyamoya patients.
- Valproic Acid (Depakote). It is another option for managing seizures.
7. Statins.
Statins are used to lower cholesterol levels, which can help reduce the risk of atherosclerosis and potentially lessen the burden on the cerebrovascular system. Examples include:
- Atorvastatin (Lipitor). This is a widely used statin that helps manage cholesterol levels.
- Simvastatin (Zocor). Zocor is commonly prescribed statin for the same purpose.
8. Pain Relief Medications.
They are indicated to manage headaches and discomfort that may be associated with Moyamoya Disease. Examples include:
- Acetaminophen (Tylenol). This is commonly used for pain relief.
- Ibuprofen (Advil, Motrin). It is an NSAID that may also be used for pain and inflammation.
9. Experimental Therapies.
Some experimental drugs and treatments are being explored for their potential benefits in Moyamoya Disease, although these are not yet widely accepted or approved. Examples include:
- Endothelial Progenitor Cell Therapy. It is being researched as a way to promote the formation of new blood vessels in the brain.
Surgical Interventions
- Direct Bypass Surgery. This procedure involves connecting a healthy artery (often from the scalp) directly to the brain’s surface. It provides an immediate improvement in blood flow to the affected areas of the brain.
- Indirect Bypass Surgery. This technique involves placing a flap of tissue over the brain or connecting it to the brain’s surface to promote the growth of new blood vessels. This method is less invasive and can be used in cases where direct bypass is not feasible.
Lifestyle Modifications
- Manage the Risk Factors. One major way of preventing the development of Moyamoya disease is controlling other chronic illnesses. Patients are encouraged to adopt a heart-healthy lifestyle, including regular exercise and a balanced diet. These activities may help in controlling risk factors such as high blood pressure, diabetes, etc.
- Avoiding Stroke Triggers. Activities that increase the risk of stroke, such as high-impact sports or strenuous physical activities, should be minimized. Check more treatment options here: https://shorturl.at/cPOAx
Living with Moyamoya Disease
Living with Moyamoya Disease requires ongoing management and lifestyle adjustments such as:
Adhering to Treatment Plans
Consistent adherence to prescribed treatments and regular follow-up appointments with a neurologist is essential. This ensures that any changes in the condition are promptly addressed and that treatment plans are adjusted as necessary.
Healthy Lifestyle Choices
- Balanced Diet: A diet rich in fruits, vegetables, whole grains, and lean proteins supports overall health and helps manage risk factors.
- Regular Exercise: Engaging in moderate exercise, as recommended by healthcare providers, can improve cardiovascular health and overall well-being.
Stress Management
Managing stress is important for overall health and can help reduce the risk of stroke. Techniques such as mindfulness, meditation, and gentle physical activities like yoga can be beneficial. Here are more tips you can use while living with Moyamoya disease: https://shorturl.at/JJmUA
Frequently Asked Questions (FAQs)
1. What is Moyamoya Disease?
Moyamoya disease is a rare brain disorder where arteries at the base of the brain become narrowed, leading to strokes or mini-strokes.
2. What are the Symptoms of Moyamoya Disease?
Symptoms include recurrent strokes, severe headaches, seizures, and weakness on one side of the body.
3. How is Moyamoya Disease Treated?
Treatment often involves surgery to improve blood flow to the brain, reducing the risk of strokes.
4. Does Moyamoya Disease Have a Cure?
Moyamoya disease has no cure, but surgical treatments can manage symptoms and reduce the risk of strokes.
5. Who is at Risk of Developing Moyamoya Disease?
People with certain genetic conditions, such as Down syndrome or neurofibromatosis, are at higher risk, but Moyamoya can also occur in individuals without these conditions.